Constipation: What Can We Do About It?
By Katie Ruebush PT, DPT
What is Constipation?

- Bloating
- Abdominal pain
- Rectal pain
- Pelvic pressure
- Hard, small stools that require pushing and straining to eliminate
If you’ve ever been constipated, these symptoms might sound familiar. Nothing feels good when you aren’t pooping on a regular basis.
Here’s the deal–constipation can be the root of lots of pelvic health symptoms. Besides the gross feeling we get when we haven’t pooped for several days, constipation makes urinary frequency, urgency, and leakage worse. It can also make pelvic pain, abdominal pain and possibly back pain worse. Resolving constipation typically improves other pelvic symptoms.
Here are some helpful tips to resolve this uncomfortable situation.
1. Drink adequate water and eliminate foods and beverages that are dehydrating/slow digestion
2. Avoid water additives, caffeine and alcohol
3. Avoid processed foods, dairy and foods containing white flour
4. Increase your water intake
- Ideally 64 oz per day
5. Eat a diet higher in fibre while drinking plenty of fluids
6. Stay active
- Physical activity improves bowel motility
- Walk, bike, do some resistance training, anything to encourage movement
7. Try a self-abdominal massage
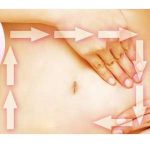
- Start on the lower right side of the pelvis
- Using 2 fingers, make small gentle circles with mild pressure around to the top of the rib cage
- Skip the middle 2 inches of the upper abdomen where the aorta lies
- Resume the small circles on the left side and down to the lower left side of the pelvis
- End at the lower abdomen near the center of the body and near the pubic bone
- Make 5 to 8 complete circles around the abdomen
- This is meant to follow the path of the large intestine
*Remember to skip the upper middle two inches to avoid compressing the aorta
8. Use proper pooping posture
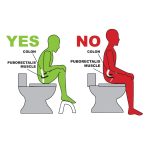
- Place your feet on a stool with knees higher than hips and slightly lean forward–this puts the rectum in an optimal position to empty
- Relax
- No straining or pushing (this puts more pressure on the pelvic structures and can cause more problems)
- Try some deep breathing to avoid straining and pushing.
- Give it time, sit on the toilet for several minutes to make sure you are allowing time to fully empty your bowels
- Try sitting on the toilet after meals even if you don’t have to go (This is typically a time when the colon is stimulated and might be ready to empty)
9. Use stool softeners or natural laxatives as directed by your doctor
10. RELAX the pelvic floor muscles
- A tight/overactive pelvic floor muscle can contribute to constipation
- A specific pelvic floor muscle wraps around the rectum and when overactive ,can prevent the release of feces
- Find 5-10 minutes, 1-2 times per day just to RELAX the pelvic muscles
- Lay on your back, knees propped up on pillows
- Spread your knees apart and point them outward
- Think about relaxing your hips, buttocks, abdomen and pelvic floor muscles
- Cues for pelvic floor relaxation include “opening”, thinking about the feeling just before you urinate
- The pelvic floor can be thought of as an “elevator”, where contracting would be the elevator rising and relaxing would be the elevator lowering
- Try to make your pelvic floor muscles “Drop, sink, and melt”
11. See a pelvic floor physiotherapist
- For specific, individualized treatments
- This can include manual therapy techniques, exercises, stretches and various modalities
Here’s to getting your gut moving!
Katie
For more information, contact www.physiopharm.company
Online consulting available. Use the code NEW for 10% off.

