Dr. Curtis Nickel’s Clinical Recipes for Success in Managing IC/BPS
What Is Interstitial Cystitis and Bladder Pain Syndrome?
Interstitial cystitis (IC), also known as bladder pain syndrome (BPS), is a chronic condition that affects the bladder and surrounding tissues. It is characterized by recurring episodes of pelvic pain, discomfort, and pressure in the bladder and urinary tract, and can cause a frequent and urgent need to urinate.
Although the exact cause of IC/BPS is not fully understood, it is believed to be related to inflammation or damage to the bladder lining. Some possible causes of IC/BPS may include genetic factors, autoimmune disorders, or chronic infections.
Treatment for IC/BPS is aimed at managing symptoms and improving quality of life. There is no cure for IC/BPS, but several treatment options are available, including bladder instillations, pelvic floor physical therapy, medications, and nerve stimulation. Lifestyle changes, such as avoiding certain foods or beverages that may irritate the bladder, may also help to reduce symptoms.
Dr. Curtis Nickel’s Clinical Recipes for Success
One of the leading global key opinion leaders within the space of inflammatory disease and infection of the urinary tract is Dr. Curtis Nickel, a member of the Department of Urology at Queen’s University since 1984.
In December 2022, the Canadian Urological Association Journal published Dr. Nickel’s latest article Managing interstitial cystitis/bladder pain syndrome in female patients: Clinical recipes for Success.
After explaining the base treatments and screening tactics for IC/BPS, Dr. Nickel extrapolates key trends and patterns that he has witnessed throughout his years as a urologist and researcher. Through those trends, he created 9 distinct phenotypes or categories of IC/BPS patients, so that in his words “the correct ingredients for a personalized management recipe” can be chosen (table 1).
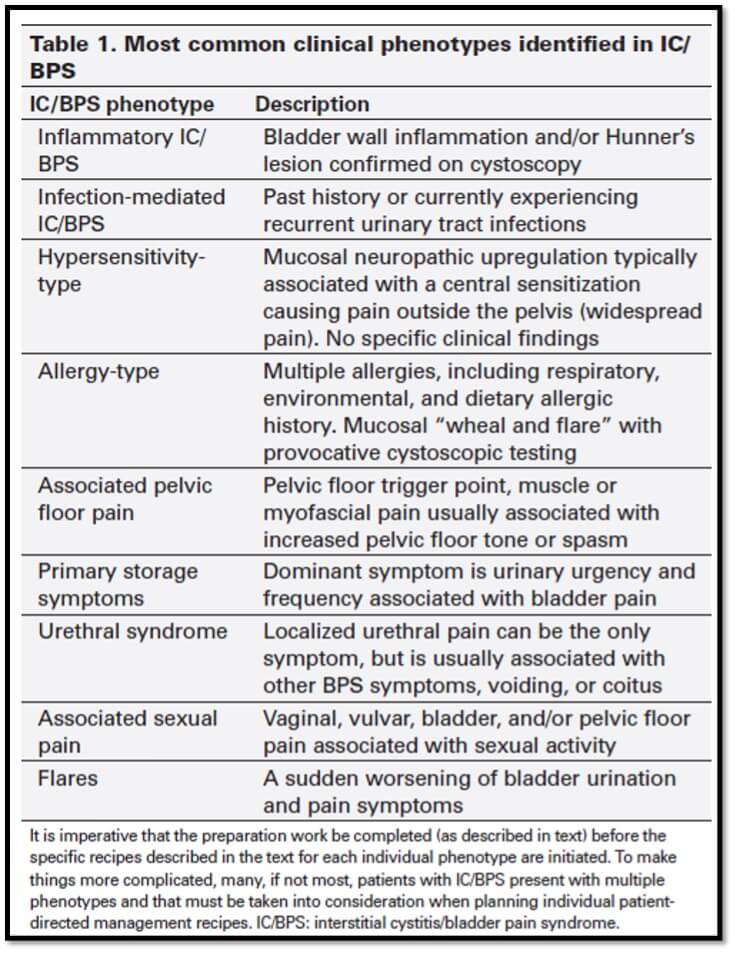
The article details his various recommendations for treatment dependent on the 9 patient phenotypes he established throughout his experience. What is interesting to note is that for 5 out of the 9 phenotypes, Dr. Nickel recommends the use of glycosaminoglycan bladder instillations, which consist of hyaluronic acid, heparin, and chondroitin sulfate (table 2). It is believed that supplementing an abnormal GAG layer in the IC/BPS bladder promotes both protective and anti-inflammatory mechanisms, leading to amelioration of bladder specific symptoms.
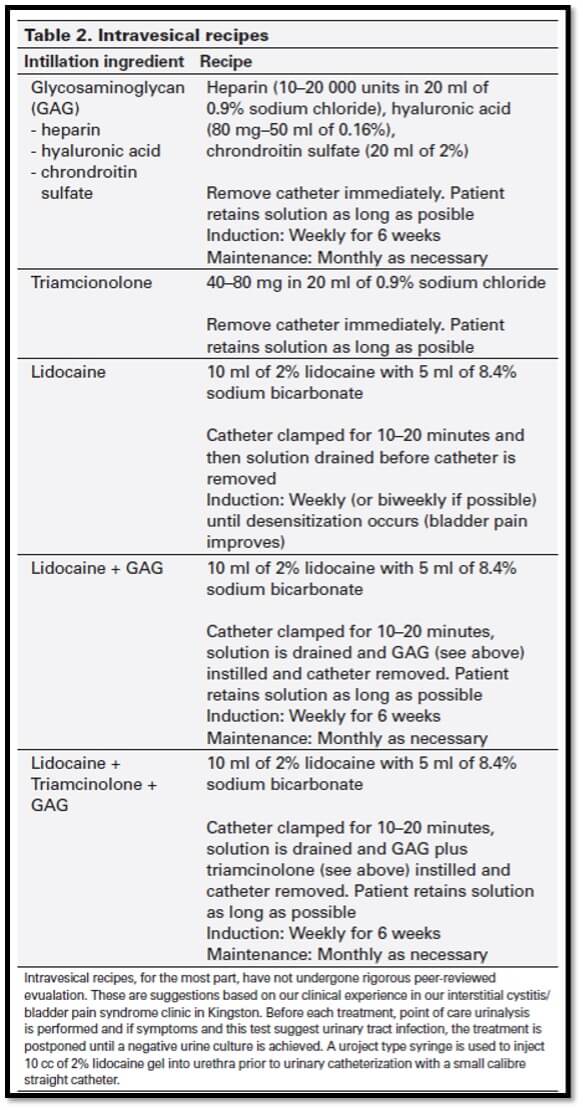
The Benefits of Hyaluronic Acid
When analyzing Dr. Nickel’s Phenotypes and recipes for each, one can see that hyaluronic acid plays a key role in 5 out of the 9 treatment processes.
With interstitial cystitis and bladder pain syndrome (IC/BPS), the bladder lining is often damaged or inflamed, which can lead to a loss of the protective layer that lines the bladder (GAG Layer). This can result in increased exposure of the underlying tissues to irritants in the urine, leading to pain, discomfort, and inflammation.
Hyaluronic acid may be beneficial for people with IC/BPS because it can help to restore the protective layer of mucus in the bladder lining. It works by binding to water molecules and forming a gel-like substance that helps to maintain tissue hydration and lubrication. This can help to protect the bladder lining from irritants.
The Canadian Urological Association has recommended Hyaluronic Acid as a grade C option for treatment of IC/BPS. In addition, the European Urological Association has recommended Hyaluronic Acid as an option to treat recurrent urinary tract infections.
INSTYLAN: Allowing Bladder Instillations in the comfort of your home
INSTYLAN is a hyaluronic acid solution with packaging that enables instillation at home through a catheter. The packaging also encompasses an additional port, allowing for the addition of other drugs, such as heparin, and chondroitin sulfate based on physicians’ recommendations (up to 50 ml). In doing so, INSTYLAN provides capability to treat 5 of the 9 phenotypes established by Dr. Nickel.
For more information on INSTYLAN, visit the web site or call 1-877-563-7422.
Dr. Nickel’s Live Q & A
We are pleased to announce that Dr. Curtis Nickel will be joining Pelvic Health Support founder, Marnie Glavin for a live YouTube Q&A session on Thurs, May 25th at 8pm EST. Dr. Nickel will be discussing his experience working with IC/BPS patients, the discoveries he has made surrounding bladder instillations and the intravesical agent recipes he has established. Following the discussion, we will open the floor to questions.
The session will be taking place on the Pelvic Health Support YouTube channel. Please subscribe to ensure notifications of the session.
We look forward to seeing you there!
References:
Cox, A., Golda, N., Nadeau, G., Nickel, J. C., Carr, L., Corcos, J., & Teichman, J. (2016). CUA guideline: Diagnosis and treatment of interstitial cystitis/ bladder pain syndrome. Canadian Urological Association Journal, 10(5-6), E136–55. https://doi.org/10.5489/cuaj.3786
Bonkat (Chair), R. Bartoletti, F. Bruyère, T. Cai, S.E. Geerlings, B. Köves, S. Schubert, A. Pilatz, R. Veeratterapillay, F. Wagenlehner. EAU Guidelines on Urological Infections. presented at the EAU Annual Congress Amsterdam, the Netherlands 2022. ISBN 978-94-92671-16-5.
Nickel, J. C. (2022). Managing Interstitial Cystitis/Bladder Pain Syndrome in the Female: Clinical Recipes for Success. Canadian Urological Association Journal, 16(12), 393-8.
Wyndaele, J. J. J., Riedl, C., Taneja, R., Lovász, S., Ueda, T., & Cervigni, M. (2019). GAG replenishment therapy for bladder pain syndrome/interstitial cystitis. Neurourology and urodynamics, 38(2), 535-544.

